Ketosis Dynamics Management.
Throughout the evolution of humanity ketosis has been naturally selected for our survival, development and protection, until today. It takes hard work (and “civilization” endorsed by the medical industry ) to avoid being in ketosis. Today almost everything in the civilized world conspires to kick us out of ketosis and towards chronic disease. The modern world of convenience, plenty and comfort is not our ally in health matters and neither are pharmaceutical drugs. We need to be conscious, aware and capable of ketosis dynamics management.
Ketosis, on a cellular level, refers specifically to the metabolism of ketones in the mitochondria. It is a relatively recent evolutionary adaptation that is found only in amniota (All reptiles, birds and mammals) (ref 8). Ketosis is why birds can migrate half way around the world without resting. It’s why people can live well even in the Arctic, hunt for food while not eating and outrun over distance practically all other animals.
Globally we can state that ketosis is when the primary fuel system in the body is fat metabolism.
In practical terms ketosis is slightly more complicated to define. Ketosis is really a dynamic system that requires management. There are three main aspects to ketosis dynamics management:
- Measuring ketones
- Generating Ketones
- Metabolizing Ketones
Tim Noakes has for a long time been regarded as one of the leading scientific authorities on sports nutrition. He actually invented the very first sports Gel supplement and overwhelmingly advocated high carbohydrate use… until he ended up himself with diabetes type 2 despite running over 70 marathons and ultra trails. He openly admits his huge errors and now strongly advocates a high fat,low carb diet.
1. Measuring Ketones
The body is always manufacturing some ketones. A few serious illnesses actually cause too many ketones to be made (notably type 1 diabetes and liver damage from alcoholism (18 mmol/l +) ). Normal health makes excessive ketone production impossible and there is no risk at all from the acute problems of “ketoacidosis”. There is however a potentially fatal risk of long term chronic disease if ketone production is kept near the “zero” end of the scale – which is the most common scenario in the developed world today.
Measuring ketones alone doesn’t tell you much. A Type 1 Diabetic can have very high levels of ketones but it’s because they cannot be metabolised at a cellular level. A healthy person can have a high level due to carbohydrate dependence because they can only consume ketones in the brain and heart and not in the muscles. Someone with an optimal metabolism will still vary a great deal during a day depending on eating, fasting and exercise habits.
There are three routes to measuring ketones at any instant; blood, urine or breath.
Beta-hydroxybutarate is the ketone tested for in the blood: (probably because type 1 diabetics have mainly beta-hydroxybutarate)
Basal ketone level 0.0 to 0.5 mmol/l
Light ketone level 0.5 to 1 mmol/l
Medium ketone level 1 to 3 mmol/l
High ketone level 3 to 6 mmol/l (I’ve seen healthy breath measurement at 7.2 mmol/l (1.3 g/l))
Acetoacetate is the ketone measured in urine. It is known to correlate very well with blood measurements at low levels but to be inaccurate at high levels. (ref 17)
Acetone is the ketone measured in breath. Once again, not as consistent as blood testing and very dependent on the specific device used. Still, it gives a repeatable result that can very inexpensively provide reasonable feedback.
Here is a link to an extremely inexpensive Chinese breath testing device that works for ketones: Tester
If the link has stopped working the image below is what it should look like when you find another source. The only reason this works is because it has a cheap microchip sensor that cannot tell the difference between acetone and alcohol. More expensive breath testers will not work for acetone. “BAC” actually refers to Breath Alcohol Content – but for our purposes we can refer to Breath Acetone Content (though there is no actual calibration for acetone).
mmol/l = g/l = BAC
0,5 = 0,09 = 0.009%
1,0 = 0,18
1,5 = 0,27
2,0 = 0,36
2,5 = 0,45
3,0 = 0,54 = 0.054%
3,5 = 0,63
4,0 = 0,72
4,5 = 0,81
5,0 = 0,90
5,5 = 0,99 = 0.099%
6,0 = 1,08
6,5 = 1,17
7,0 = 1,26
7,5 = 1,35 = 0.135%
2. Generating Ketones
Ketosis is the body’s primary metabolic state so it should come as no surprise that there are many factors involved in controlling it. Ketosis is NOT a “starvation” mode or any such nonsense. If your lifestyle is healthy then you are automatically in ketosis. If you are not in ketosis then your lifestyle is probably not optimum for good health.
There is a huge degree of bio-individuality between people within any race. Making sweeping generalities risks failing to respect biological differences. However, the medical/pharmaceutical industrial complex does not hesitate to endorse the fatally false and damaging notion that glucose dependence is normal. If by chance my declaration that ketosis is the real “normal” goes a little too far – then I’m very glad to err in that direction.
Main Synergetic Factors in Ketone Generation
- Exercise
- Fasting – Intermittent fasting
- Ketogenic nutrition
- MCT foods
- Microbiome
- Exogenous ketones
- Cold exposure
- Nasal breathing
- Bio-individuality
There is a synergy for ketosis between the various factors and between the components comprised within each factor.
Exercise

Moderately intense exercise for 90 minutes or longer will raise ketone levels by between 0.5 and 2.0 mmol/l.
There’s unlikely to be a noticeable increase during exercise due to that fact that ketones are being rapidly metabolized, though the level should rise post exercise.
Fasting – Intermittent Fasting
Fasting for 2 days for a woman and 3 days for a man (starting from having eaten mainly carbohydrates) will raise ketone levels, probably to 2.0 or 3.0 mmol/l. The level will continue to rise steadily if the fasting continues for longer periods, easily reaching 6 or 7.0 mmol/l.
Intermittent Fasting can be sustained indefinitely and help reach and maintain a high level of ketosis when combined with ketogenic nutrition and exercise. There’s various concepts of intermittent fasting such as one (or more) 24 hr period per week, or 36 hrs or 48 hrs. Instead, you can divide each day (or some days) into a ratio such as 6/18 where you can only eat in the 6 hour period. 8/16 ratio works too. If you maintain steady ketosis that that will effectively protect you from muscle loss while fasting.
Ketogenic Nutrition
A diet based on approximately 70% of Calories (not weight!!!) from appropriate fats, 20 % from protein and 10% from carbohydrates. This is essential for long term stability of ketosis. We will look at ketogenic nutrition in detail in the following articles. Too much carbohydrate or too much protein will reduce or stop ketosis.
MCT Medium Chain Triglycerides
Certain fats are high in Medium Chain Triglyceride (MCT) content. Coconut fat and Palm oil are examples. MCTs cannot be stored as fat in the body. They are delivered directly to the liver for conversion into ketones. MCTs are defined as having from 6 to 12 carbon atoms.
Coconut fat is 60 to 70% MCT. (Only buy organic, non deodorised, cold pressed.)
MCT Fatty acid content of Coconut Oil and Palm Oil (ref 15)
| Coconut | Palm | Formula | |
| Caproic | 0.5% | 0.3% | C6H12O2 |
| Caprylic | 7% | 4.9% | C8H16O2 |
| Capric | 8% | 4.6% | C10H20O2 |
| Lauric | 48% | 47.5% | C12H24O2 |
Microbiome
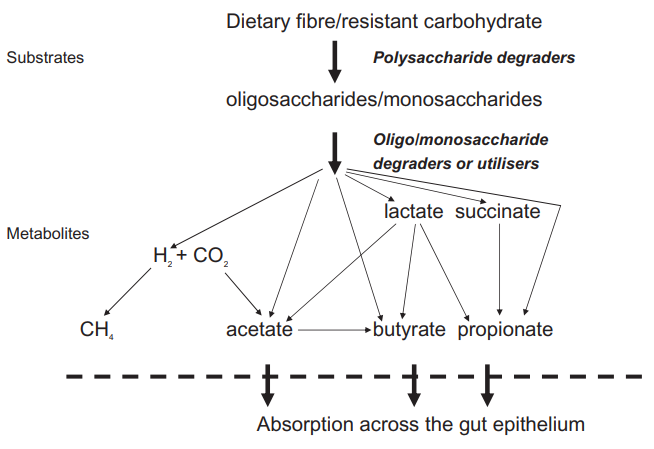
Ketone production gets a strong boost from dietary fibre. The term “dietary fibre” is very misleading. It’s an umbrella term for any carbohydrate that can’t be digested in the upper tract of the intestine – meaning that you can’t break it down. Perhaps a better term is “prebiotic”.
Let’s begin by eliminating “insoluble” dietary fibre which shreds your colon and should be thoroughly avoided. We need soluble dietary fibre. This type of carbohydrate is only digested by the bacteria in your gut. It literally feeds the gut’s symbiotic microbes (anaerobic fermentation) and the bacteria in turn supplies you with byproducts which are valuable nutrients. You absorb those nutrients through the wall of the intestine.
We’ll look at two of the most important prebiotics; inulin and fucose.
Inulin is a polysaccharide (dietary fibre/fructan) and the diagram here shows the stages by which it is broken down into Short Chain Fatty Acids (SCFAs) of which butyrate is the most predominant. (For some illogical reason they are not named Short Chain Triglycerides – having less than 6 carbon atoms.)
While inulin increases beneficial bacteria, including Bifidobacterium and Lactobacillus-Enterococcus the butyrate they produce adversely affects pathogenic bacteria like Escherichia coli, Salmonella spp., and Campylobacter spp. (ref 18)
Butyrate itself can undergo β-oxidation, a mechanism for ketone production.
Here is a list of the main benefits and functions of butyrate (ref 16 &18) :
- Induces FGF21 in serum, liver, and adipocytes, which in turn stimulates fatty acid β-oxidation and hepatic ketone production
- Induces GLP-1 secretion (glucose tolerance and appetite control)
- Stimulates neurogenesis via brain derived neurotrophic factor (BDNF) upregulation
- Antidepressant effect
- Obesity management – remaining lean (despite dietary calorie load) with increased energy expenditure in the form of body heat generation (FG21 – browning of WAT) and a tendency to be more physically active. (WAT is White Adipose Tissue)
- Better insulin sensitivity
- Improves cardiac health with lower cholesterol production
- Improves gut lining integrity
- Neuroprotection and improved memory recall in Alzheimer’s disease
- Provides improved long-term inflammatory control, including Crohn’s disease
- Reduces propionic acid-producing microbes (Propionic acid is implicated in Autism Spectrum Disorders(ASD))
- Maintains healthy peristalsis (movement of food in the digestive tract)
Fucose is an oligosaccharide which is found in abundance in brown seaweed (including kelp) and human breast milk. When fucose is fermented by the symbiotic gut microbes about the same amount of butyrate is generated as for inulin (and much higher propionate).
Fucose is known to inhibit the proliferation of melanoma cells and to induce apoptosis (programmed cell death) – which appear to be additional advantages over inulin. (ref 21)
I found out about fucose due to thinking about how our ancestors would have been living almost exclusively in ketosis, definitely eating lots of fish (30 to 40% of the brain’s “grey matter”- is Omega 3 DHA). (ref 25) To keep their gut microbiome healthy they would have to also eat prebiotic dietary fibre – so what could they eat? Seaweed obviously. Then it came as a surprise to see that the prebiotic in seaweed is “fucose” and that human milk is unusually high (about 0.5%) in fucose concentration.
One lesson from this is that anyone using ketogenic nutrition should be feeding their microbiome with either inulin, fucose or resistant starch. (Seaweed and green bananas are useful for that!)
“Tamzyn Murphy Campbell BSc, BSc Med(Hons) Human Nutrition and Dietetics, RD
Did you know that human newborns and exclusively breastfed babies are in ketosis? 1 I am a dietitian, with two years of intensive postgraduate training in nutrition, and I didn’t realise this until just over a month ago. The fact that human babies are naturally in ketosis is an inconvenient truth because it implies that ketosis (which also occurs when fasting or eating a low-carbohydrate, high-fat diet) is not only a natural metabolic state for human infants, but that it’s probably beneficial too. Nature seldom does something without a reason, so it’s likely that ketosis may confer some kind of evolutionary advantage to human infants. Research suggests that it may be one of the main factors behind the development of the large human brain. “
“Babies thrive under a ketogenic metabolism
Some people, even some scientists who study ketogenic metabolism, have the idea that ketogenesis is somehow abnormal, or exceptional; an adaptation for emergencies only.
We disagree.
One reason we think a ketogenic metabolism is normal and desirable, is that human newborns are in ketosis. Despite the moderate sugar content of human breast milk, breastfeeding is particularly ketogenic. This period of development is crucial, and there is extensive brain growth during it. Although the composition of breast milk can be affected by diet, it is reasonable to assume that breast milk has always been ketogenic, and this is not an effect of modernisation.
When the brain is in its period of highest growth, and when the source of food is likely to be close to what it evolved to be for that period, ketones are used to fuel that growth.” (ref 20)
Exogenous Ketones
Various ketone sources exist naturally in our food supply.
Dairy milk contains levels ranging from 10 to 631 μM, making dairy products a natural source of β-hydroxybutyrate – albeit very small. (ref 26)
There are manufactured exogenous ketone supplements on the market now, with pro cyclists apparently spending as much as $100 per day to put them in their drinks. They appear to use them for “glucose sparing” and perhaps to get some of the anti-inflammatory and recovery benefits.
The heart can use any fuel source provided but when ketones are available all other energy substrates are pushed aside. It is estimated that the heart functions 27% more efficiently on ketones compared to glucose and fatty acids. If exogenous ketones are available in the bloodstream then they will definitely be used so it seems that there should be a measurable advantage in sports performance. (ref 27)
Only time will tell if there are problems associated with this relatively unnatural intervention. My feeling meanwhile is to stick with the natural processes and aim for an optimal metabolic state where you create your own ketones.
Cold Exposure
When a baby is born it is unable to shiver to stay warm. Nature protects the baby by providing it with an abundance of “brown fat”. Brown fat is unique in that its mitochondria directly use ATP to provide heat for the body. Adults generally do not have much brown fat, though there is a great deal of bio-individuality in this respect. Those with more brown fat tend to be thinner and have less need of warm clothing. Conversely, we now know that both endurance exercise and constant exposure to the cold increase brown fat levels.
Certain white adipose tissue (WAT) depots are readily able to convert to a “brown-like” state with prolonged cold exposure. (ref 19) Endurance exercise does this too – through an intermediary hormone called irisin (discovered 2012). Butyrate also leads to this effect (uncoupling in the mitochondria – meaning the ATP is just used for heat production) Yes, I’m pointing out the synergy between different modes of ketone generation. Cold stress, exercise and butyrate stimulate chains of hormonal effects that lead to adaptations in the mitochondria and to increased fat metabolism and ketone generation. (ref 22)
Norepinepherine is released in the brain during and after cold exposure, which improves mood and the sense of well being. Breathing techniques (hyperventilation followed by apnea) can also be used to increase adrenaline and maintain a stable core temperature. (ref 23)
Nasal Breathing
Nasal breathing, due to restricting breathing rate, increases CNS (central nervous system) tolerance to CO2. The body is trained to accept higher concentrations of CO2 dissolved in the blood. CO2 level is the trigger for the release of oxygen from the blood into the body and brain’s tissues. Raising the CO2 threshold allows more efficient and thorough tissue oxygenation. Improved oxygenation permits more efficient mitochondrial function. Nitrogen oxide (NO) is released from the rear of the nasal passages when nasal breathing. NO is vasodilatory and so is CO2 so they combine to improve blood flow. Improved mitochondrial metabolic performance enhances fat burning and encourages ketone production.
Bio-individuality
We always hear about “normal ” attributes and conditions regarding our biology – but nothing could be more deceptive and misleading. Bio-individuality yields a HUGE variation of practically every parameter measurable. The “norm” often just simply isn’t normal. People have vastly different shaped and positioned internal organs, different nerve distributions and different arterial configurations. Needless to say we have different metabolic systems too. Some people can function well and remain healthy on high carbohydrates. There are general trends regarding ancestral geography and evolution that might indicate tendencies. However, whether we look at the Polynesian islands or the USA we see the common ravages of the modern diet – obesity, diabetes, heart disease, cancer and dementia. For this reason the “big picture” has to be kept in mind and ketosis viewed as being fundamental.
The main issue here concerning ketone generation is how much glucose the individual can tolerate before ketones are suppressed. Some people can only generate a high level of ketones when carbohydrates are almost totally eliminated – (perhaps only 10 or 20 grams per day max). Others can tolerate much more carbohydrate and remain in ketosis. It’s next to impossible to gauge how much of this is biochemical individuality and how much is due to ketosis dynamics management – and that includes the metabolizing of ketones (…next article.) (ref 24)
References for all of the keto series:
- https://www.cell.com/trends/endocrinology-metabolism/fulltext/S1043-2760(13)00156-2
- Jeff S. Volek, Daniel J. Freidenreich, Catherine Saenz, Laura J. Kunces, Brent C. Creighton, Jenna M. Bartley, Patrick M. Davitt, Colleen X. Munoz, Jeffrey M. Anderson, Carl M. Maresh, Elaine C. Lee, Mark D. Schuenke, Giselle Aerni, William J. Kraemer, Stephen D. Phinney. Metabolic characteristics of keto-adapted ultra-endurance runners. Metabolism, 2015; DOI: 10.1016/j.metabol.2015.10.028
- https://www.ncbi.nlm.nih.gov/books/NBK26882/
- https://www.sciencemag.org/news/2012/01/first-oxygen-users
- https://bio.libretexts.org/Bookshelves/Introductory_and_General_Biology/Book%3A_Introductory_Biology_(CK-12)/5%3A_Evolution/5.5%3A_Evolution_of_Eukaryotes
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3957730/
- https://en.wikipedia.org/wiki/Ketone
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4176946/
- https://www.cell.com/cell-metabolism/pdf/S1550-4131(16)30355-2.pdf
- Survival of the Fittest – Mike Stroud
- Michael Pollan “The Omnivore’s Dilemma”
- http://www.thesallyedwardscompany.com/sallyedwards/sally-edwards-news.php?article=8
- https://www.triathlete.com/2019/02/nutrition/the-greatest-nutrition-lessons-of-dave-scotts-career_353431
- https://www.em-consulte.com/en/article/80600
- https://academic.oup.com/fqs/article/3/2/61/5475954
- https://juniperpublishers.com/crdoj/pdf/CRDOJ.MS.ID.555746.pdf
- https://onlinelibrary.wiley.com/doi/pdf/10.1111/j.1467-3010.2008.00706.x
- https://www.researchgate.net/publication/324157111_Potential_Synergies_of_b_-Hydroxybutyrate_and_Butyrate_on_the_Modulation_of_Metabolism_Inflammation_Cognition_and_General_Health
- http://genesdev.cshlp.org/content/26/3/271.full
- http://www.ketotic.org/2014/01/babies-thrive-under-ketogenic-metabolism.html
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3280569/
- https://books.google.fr/books?id=PmMhBQAAQBAJ&pg=PA79&lpg=PA79&dq=cold+exposure+ketone+levels&source=bl&ots=sboucv9-0L&sig=ACfU3U02xcUHb9Cwi1dn4_muhS-rlC24mg&hl=en&sa=X&ved=2ahUKEwj7i6zN5oTlAhXJxYUKHXFqBhUQ6AEwBnoECBEQAQ#v=onepage&q=cold%20exposure%20ketone%20levels&f=false
- https://podcastnotes.org/2018/07/03/attia-patrick/
- https://www.amazon.com/Biochemical-Individuality-Roger-Williams/dp/0879838930/ref=sr_1_1?keywords=biochemical+individuality&qid=1570277237&sr=8-1
- https://content.iospress.com/articles/journal-of-alzheimers-disease/jad150777
- https://www.researchgate.net/publication/7837002_Fluorometric_Determination_of_b-Hydroxybutyrate_in_Milk_and_Blood_Plasma
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5313038/
- note: While animal cells readily convert sugars to fats, they cannot convert fatty acids to sugars. (But they can convert them to ketones)
- note: Acetyl-CoA can be converted into pyruvate and lactate (lactic acid) through the ketogenic pathway.
- note: oxaloacetate is made from pyruvate (from glucose) but pyruvate itself is a ketone (though this fact is usually never mentioned